Oesophageal Cancer
Oesophageal cancer is a disease in which malignant (cancerous) cells form in the tissues of the oesophagus, the tube that carries food from the mouth to the stomach. It can cause symptoms like difficulty swallowing, chest pain, weight loss, and persistent heartburn (indigestion).
Jump to:
Introduction
Did you know? Oesophageal cancer affects over 9,000 people in the UK each year. Receiving a diagnosis can feel overwhelming, and it’s natural to have many questions about what lies ahead. Living with oesophageal cancer is a journey that involves not only medical treatment, but also emotional strength and everyday adjustments. We offer clear, compassionate information, helping you better understand your condition and the options available to you. Below, you’ll find:
- What oesophageal cancer is and how it can affect your body
- Common signs and symptoms, and why early detection matters
- Practical lifestyle and dietary tips to support your overall well-being,
including managing swallowing difficulties - Information about treatments, including surgery, chemotherapy,
radiotherapy, targeted therapies and immunotherapy - Guidance on managing side effects such as difficulty swallowing and
maintaining quality of life during and after treatment - Nutritional support strategies to help you maintain strength and weight
- Support resources for you and your loved ones, so you never feel alone in
your journey
Our goal is to give you knowledge and reassurance, so you can feel more confident when talking with your healthcare team and making decisions about your care.
Please remember: the information in this below is for guidance only and is not a substitute for professional medical advice. Always consult your healthcare team for advice tailored to your personal situation.
Watch this video explaining the causes, symptoms, diagnosis and treatment options for Oesophageal Cancer.
What is oesophageal cancer?
- Oesophageal cancer is a cancer that’s found anywhere in the oesophagus,
sometimes called the gullet or food pipe. - The oesophagus connects your mouth to your stomach.
- How serious oesophageal cancer is depends on where it is in the
oesophagus, how big it is, if it has spread and your general health.
Who is more likely to get oesophageal cancer
It’s not always clear what causes oesophageal cancer. Anyone can get it, but you might be more at risk if you:
- are over the age of 75 (it’s not very common in people under 45)
- are a man
- have certain conditions, such as long-term, severe acid reflux
(gastro-oesophageal reflux disease), or Barrett’s oesophagus
Many oesophageal cancers are also linked to lifestyle. For example, you’re more likely to get it if you’re overweight, smoke or drink too much alcohol.
It’s important to be checked by a GP if your symptoms change
Symptoms
Accurately identifying the underlying cause of your symptoms is the most vital first step on your path to effective treatment.
- Over 9,000 people are diagnosed with oesophageal cancer in the UK each year
- Risk factors include persistent acid reflux, Barrett’s oesophagus, smoking,
obesity, and excessive alcohol consumption - Men are twice as likely to develop oesophageal cancer as women
- The risk of oesophageal cancer increases significantly with age, particularly
after 55
The most common symptoms of oesophageal cancer include difficulty swallowing (dysphagia) and persistent indigestion. However, oesophageal cancer can produce a wide variety of symptoms.
How to reduce your risk of getting oesophageal cancer
Do:
- try to lose weight if you’re overweight let hot drinks cool down a bit before drinking, so they do not
- damage your oesophagus
- try to cut down on alcohol – avoid drinking more than 14 units a week
- try to quit smoking
It’s important to get any symptoms of oesophageal cancer checked by a GP. Anyone can get oesophageal cancer, even if you do not think you have a higher chance of getting it.
Get Checked!
See a GP if you have:
- Persistent problems swallowing (dysphagia), especially if it’s getting worse
- Unintentional weight loss
- Persistent indigestion or heartburn that doesn’t improve with medication
- Pain or discomfort when swallowing
- Food coming back up (regurgitation)
- Persistent vomiting
- Symptoms that get worse or do not improve after 2 weeks
Get advice from 111 now if:
- You’re having difficulty swallowing and cannot eat or drink
- You’re being sick repeatedly and cannot keep food down
- You have symptoms that worry you, but are not sure where to get help
- 111 will tell you what to do. They can arrange a phone call from a nurse or doctor if you need one.
Go to 111.nhs.uk or call 111.
What happens at the GP appointment
- The GP will ask about your symptoms and how long you’ve had them.
- They may examine your neck and abdomen.
- They may arrange blood tests to check for anaemia or other indicators.
- They may refer you for an endoscopy (a camera test to look at your
oesophagus and stomach).
Referral to a specialist
If the GP suspects oesophageal cancer, you’ll receive an urgent referral (usually within 2 weeks) to see a specialist for further tests such as an endoscopy or biopsy. An urgent referral does not definitely mean you have cancer – it ensures any serious conditions are investigated quickly.
Important
These symptoms are very common and are usually caused by less serious conditions. Most people with these symptoms will not have oesophageal cancer. However, it’s essential to get them checked by a GP.
Tests and Next Steps
If the GP or specialist thinks you might have oesophageal cancer, they will probably refer you for a test to look inside your oesophagus. This test is called a gastroscopy (a type of endoscopy) or sometimes a camera test. It looks for any problems in your oesophagus or stomach, including oesophageal cancer.
During a gastroscopy:
- A long, thin, flexible tube with a small camera inside (called an endoscope) will be put into your mouth and down your oesophagus.
- A specialist will use the camera in the endoscope to look for any problems.
- A small sample of cells (called a biopsy) may be collected during the
procedure. These cells will be sent to a laboratory to check for cancer.
The test should take around 10 to 15 minutes. It should not be painful, but you might find it uncomfortable.
You may be offered things to make you more comfortable and make the test easier, such as:
- local anaesthetic spray to numb the back of your throat
- sedation – medicine given through a small tube in your arm to help you relax
A gastroscopy can also help find problems in other nearby organs. Such as the food pipe (oesophageal cancer) and the first part of the bowels (small intestine).
Getting your results
You should get the results of a gastroscopy and biopsy within 2 weeks. Try not to worry if your results are taking longer to get to you. It does not definitely mean anything is wrong.
You can call the hospital or GP if you’re worried. They should be able to update you.
A specialist will explain what the results mean and what will happen next.
You may want to bring someone with you for support.
If you’re told you have oesophageal cancer
Being told you have oesophageal cancer can feel overwhelming. You may be feeling anxious about what will happen next.
It can help to bring someone with you to any appointments you have. A group of specialists will look after you throughout your diagnosis, treatment and beyond.
Your team will include a clinical nurse specialist who will be your main point of contact during and after treatment.
You can ask them any questions you have.
Next steps
If you’ve been told you have oesophageal cancer, you will need more tests. These, along with the camera test, will help the specialists find out the size of the cancer and how far it’s spread (called the stage).
You may need:
- scans, like an ultrasound scan (sometimes from inside your body using an endoscope), CT scan, or PET-CT scan
- a small operation to look inside your tummy, called a laparoscopy
You may not have all these tests.
The specialists will use the results of these tests and work with you to decide on the best treatment plan for you.
Oesophageal cancer can be treated, but treatment is often challenging.
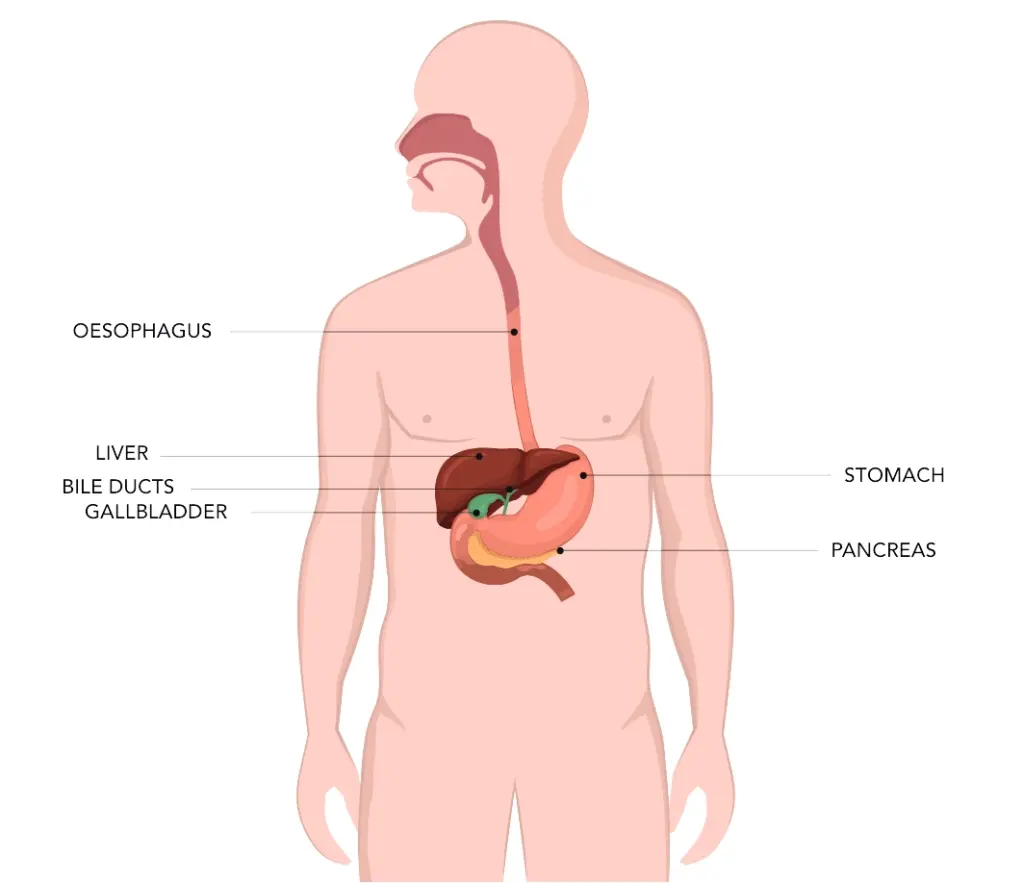
Treatments
Treatment for oesophageal cancer
Oesophageal cancer can be treated, but treatment is often challenging. The treatment you have will depend on:
- the size and type of oesophageal cancer you have
- where it is
- if it has spread
- your general health
It may include surgery, chemotherapy, radiotherapy, and targeted medicines and immunotherapy.
The specialist care team looking after you will:
- explain the treatments, benefits and side effects
- work with you to create a treatment plan that is best for you
- help you manage any side effects, including changes to your diet
You’ll have regular check-ups during and after any treatments. You may also have tests and scans.
If you have any symptoms or side effects that you’re worried about, talk to your specialists. You do not need to wait for your next check-up.
Surgery
If oesophageal cancer is found early and it has not spread, you may be able to have surgery to remove it. The surgeon will remove part or, in a small number of people, most of the oesophagus. They may also need to remove parts of other organs around the oesophagus, such as the top of the stomach.
Chemotherapy
Chemotherapy uses medicines to kill cancer cells. You may have chemotherapy for oesophageal cancer:
- before surgery to help make the cancer smaller
- after surgery to get rid of any remaining cancer and help stop the cancer
coming back - with radiotherapy (chemoradiotherapy) to treat early cancer, or if you’re not able to have surgery
- to help control and improve the symptoms of advanced cancer
Radiotherapy
Radiotherapy uses high-energy rays of radiation to kill cancer cells. You may have radiotherapy for oesophageal cancer:
- to treat early cancer, usually with chemotherapy (chemoradiotherapy)
- to help control and improve the symptoms of advanced cancer
Targeted medicines and immunotherapy
Targeted medicines and immunotherapy aim to stop the cancer growing and help your immune system attack the cancer. You might have treatment with targeted medicines or immunotherapy:
- if the cancer has spread to another part of the body
- if the cancer cannot be cured
- to lower the risk of the cancer coming back after surgery to remove it
Palliative Care
What happens if you’ve been told your cancer cannot be cured
If you have advanced oesophageal cancer it might be very hard to treat.
It may not be possible to cure the cancer. In this situation, the aim of your treatment will be to limit the cancer and its symptoms, and help you live longer.
Finding out the cancer cannot be cured can be very hard news to take in. You will be referred to a special team of doctors and nurses called the palliative care team or symptom control team. They will work with you to help manage your symptoms and make you feel more comfortable. The clinical nurse specialist or palliative care team can also help you and your loved ones get any support you need.
Information from the NHS website
https://www.nhs.uk/conditions/oesophageal-cancer/
How the OPA can help
For more than four decades, OPA Cancer charity has fought against Oesophageal and Gastric Cancers, raising awareness about the dangers of persistent hearburn (indigestion), Barrett’s Oesophagus and Gastroesophageal Reflux Disease. Wherever you are on your journey – whether newly diagnosed, undergoing treatment, or years into recovery – the OPA is here for you. From navigating chemotherapy, radiotherapy, or surgery, to offering guidance and resources, we are dedicated to providing vital information and compassionate support to those affected by these cancers.
Frequently Asked Questions
Feeling tired is common with oesophageal cancer, treatment, or after surgery. It can be caused by the cancer itself, anaemia, treatment side effects, or changes in diet.
Your healthcare team can help manage fatigue.
Prognosis varies depending on the type, stage, and treatment response. Your specialist can give the most accurate information for your situation.
Recovery from oesophageal surgery can take several weeks to months. Most people spend 1–2 weeks in hospital, followed by gradual return to normal activities at home.
Many people can return to physical activities, but it depends on your recovery and energy levels. Your doctor or physiotherapist can guide when it’s safe.
Eating may feel different after treatment or surgery. Small, frequent meals and dietary adjustments are often needed, and a dietitian can provide tailored advice.
Chemotherapy, radiotherapy, and surgery can cause side effects like nausea, fatigue, sore throat, or swallowing difficulties. Your healthcare team can help manage them.
Many people continue working during treatment, but it depends on your energy levels, type of treatment, and job demands. Your doctor can advise on adjustments or time off.
Some treatments can affect swallowing or voice temporarily. Speech and language therapists can provide exercises and strategies to improve function.
Feeling anxious, depressed, or stressed is common. Support is available through counselling, support groups, and talking to your healthcare team.
Many people benefit from home care support, dietary advice, physiotherapy, or help from family and friends. Your hospital or local cancer charity can guide you.














