Acid reflux and Oesophagitis
What is GORD?
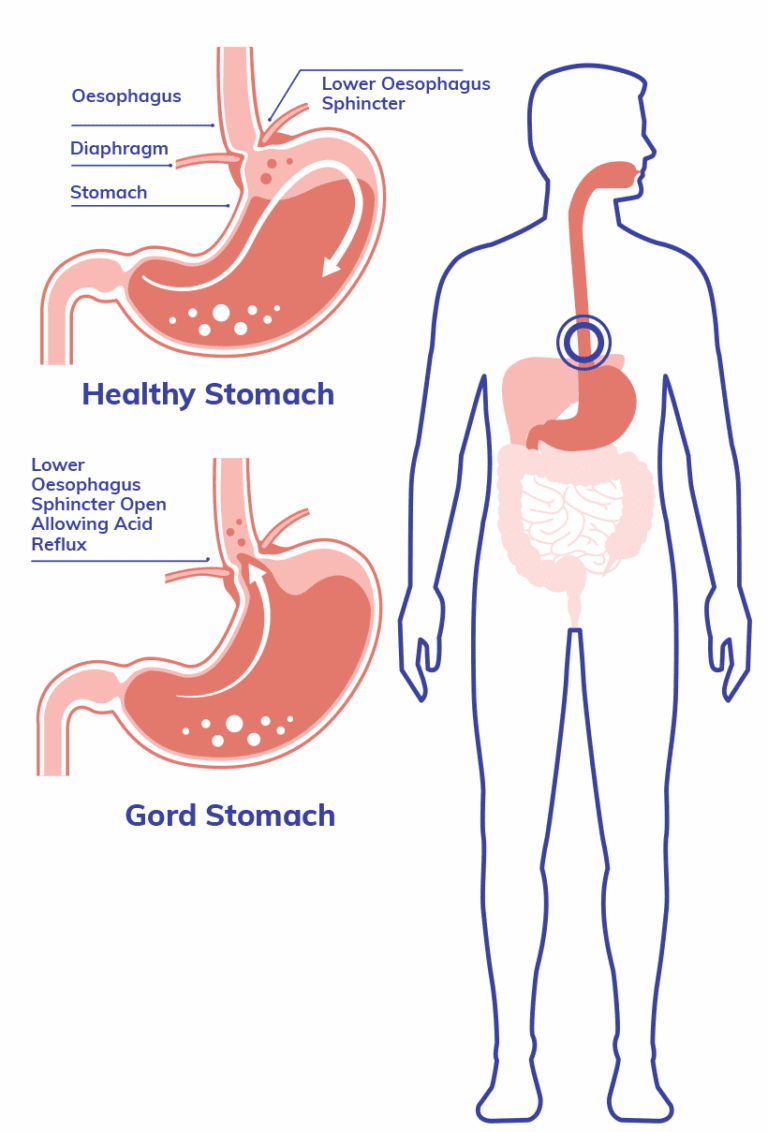
When we eat, food travels from the mouth, down the oesophagus (gullet), and into the stomach. The stomach produces acid and other substances to help digest food. It also produces mucus to protect its lining from damage by the acid. However, the cells lining the oesophagus are different and do not have the same protection.
At the point where the oesophagus meets the stomach, there is a ring of muscle known as a sphincter. This muscle relaxes to allow food to pass into the stomach, then tightens to prevent food and acid from moving back up into the oesophagus.
GORD is the term used to describe repeated episodes of acid reflux, which may or may not cause oesophagitis. It is a common condition that can lead to symptoms and discomfort if not managed properly.
What causes GORD?
GORD may develop for several reasons, including:
- A weakened sphincter muscle between the oesophagus and stomach.
- Increased pressure in the stomach that overcomes the sphincter. This can happen during pregnancy, after eating a large meal, or when bending forward.
What are acid reflux and oesophagitis?
- Acid reflux occurs when stomach acid flows back into the oesophagus.
- Oesophagitis is inflammation of the oesophagus lining, which may be caused by repeated exposure to stomach acid.
What are the symptoms of acid reflux and oesophagitis?
The most common symptom is heartburn – a burning sensation in the centre of the chest, often worse after eating or when lying down. Despite the name, heartburn has nothing to do with the heart.
Other symptoms may include:
- Feeling nauseous
- A bitter or acidic taste in the mouth
- Burning pain when swallowing
- Frequent belching
It’s important to be checked by a GP if your symptoms change
How can I manage my symptoms?
Everyone’s experience is different, but the following lifestyle changes may help alongside any medical treatment advised by your doctor.
Maintain a healthy weight
Being overweight increases pressure on the stomach and the lower oesophageal sphincter. Losing weight can significantly improve symptoms. If you need support with weight loss, speak to your GP.
Tips for losing weight:
- Make long-term, realistic changes to your diet. Avoid crash diets.
- Eat regular, small meals and don’t skip breakfast.
- Reduce sugary foods and drinks.
- Do daily physical activity – even short walks can help.
- Replace snacks with healthier options such as fruit or vegetables.
Managing night-time acid reflux
If your symptoms are worse at night:
- Avoid eating within 3 hours of going to bed.
- Try lying on your left side.
- Raise the head of your bed or use extra pillows to help keep acid in the stomach.

Avoid triggers in food and drink of getting oesophageal cancer
Certain foods and drinks can make acid reflux worse. You may benefit from reducing or avoiding:
- Caffeinated drinks (tea and coffee)
- Alcohol
- Spicy or fatty foods
- Fizzy drinks
- Chocolate
- Peppermint (including chewing gum)
- Citrus fruits and juices
- Tomatoes and onions
Try removing these from your diet one at a time to identify what affects you most. Don’t forget to drink plenty of water.
Eat smaller, more frequent meals
Eating large meals can worsen symptoms. Instead, try:
- Eating smaller amounts more frequently throughout the day
- Eating slowly
- Sitting upright during and after meals
Stop smoking
Smoking reduces saliva production and relaxes the sphincter muscle, increasing the risk of acid reflux. Quitting smoking will help relieve symptoms and improve overall health. Support is available through NHS Stop Smoking Services.
Medications
Some medicines can weaken the sphincter or irritate
the oesophagus.
These may include:
- Painkillers such as aspirin or ibuprofen
- Calcium channel blockers
- Nitrates
- Diazepam
If you suspect a medication is making your symptoms worse, do not stop taking it without consulting your doctor.
Manage stress and stay active
Try to be active on most days – aim for at least 30 minutes of moderate exercise. This can also help with weight management.
To reduce reflux when exercising:
- Avoid eating just before physical activity
- Try to eat after, rather than before, exercise
When should I seek medical advice?
Speak to your GP if:
- You experience symptoms several times a week
- Your symptoms are getting worse or more frequent
- You have difficulty swallowing
- You vomit or cough up blood
- You have lost weight unintentionally














